Abstract
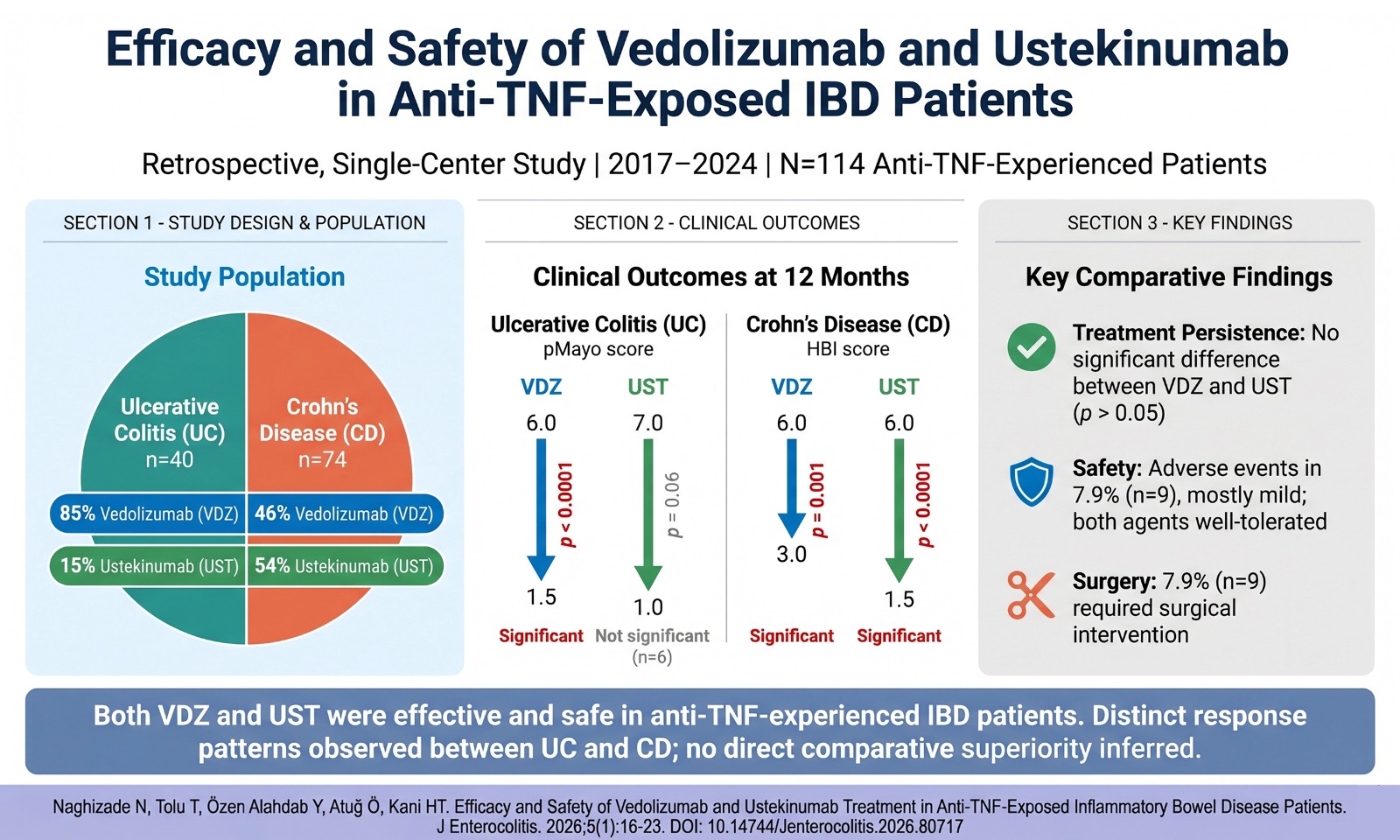
Objective: The environmental footprint of healthcare is increasingly recognized as a component of care quality; however, patient-level carbon emissions associated with inflammatory bowel disease (IBD) remain insufficiently quantified. This study aimed to prospectively quantify the carbon footprint of IBD care and compare it across major maintenance treatment strategies.
Methods: This prospective observational cohort study was conducted at a tertiary IBD referral center between December 2025 and January 2026. Consecutive adults with ulcerative colitis or Crohn’s disease were included. For each participant, the annual carbon footprint (kg carbon dioxide equivalent [CO₂e] per patient-year) was estimated using activity-based accounting based on healthcare utilization during the preceding 12 months across three domains: patient travel, clinical care delivery, and pharmaceuticals. Patients were stratified by their dominant maintenance therapy. Independent predictors were assessed using multivariable linear regression.
Results: Among 248 patients (169 with ulcerative colitis and 79 with Crohn’s disease), the median annual carbon footprint was 52.6 kg CO₂e (interquartile range, 31.8–74.2). Patient travel accounted for 46.2% of emissions, followed by pharmaceuticals (29.4%) and clinical care delivery (24.4%). The carbon footprint was highest with intravenous biologics (86.1 kg CO₂e), followed by subcutaneous biologics (48.9 kg CO₂e) and oral/systemic therapy (24.7 kg CO₂e) (P < .001). In adjusted analyses, intravenous and subcutaneous biologics were associated with increases of 31.4 kg CO₂e (95% CI, 24.1–38.7) and 18.6 kg CO₂e (95% CI, 12.2–25.1), respectively. Each 10-km increase in one-way travel distance was associated with an additional 3.2 kg CO₂e (95% CI, 1.9–4.5).
Conclusion: Long-term IBD management is associated with a measurable carbon footprint, primarily driven by treatment modality and patient travel. A more sustainable organization of care may reduce the environmental impact while preserving care standards.




 Yavuz Özden1
Yavuz Özden1